Hello...
DigiBete is your QISMET accredited, trusted self-management platform and App for the whole family and community managing Type 1 diabetes. Built by families for families, and clinically approved by NHS experts. We’re here to guide you every step of the way with resources aimed at supporting anyone up to the age of 25.

DigiBete Kids & Parents
DigiBete Teens & Parents
DigiBete Adults
Schools & Teachers
Technology
Food & Drink
Sports, Activity & Wellbeing
DigiBete App
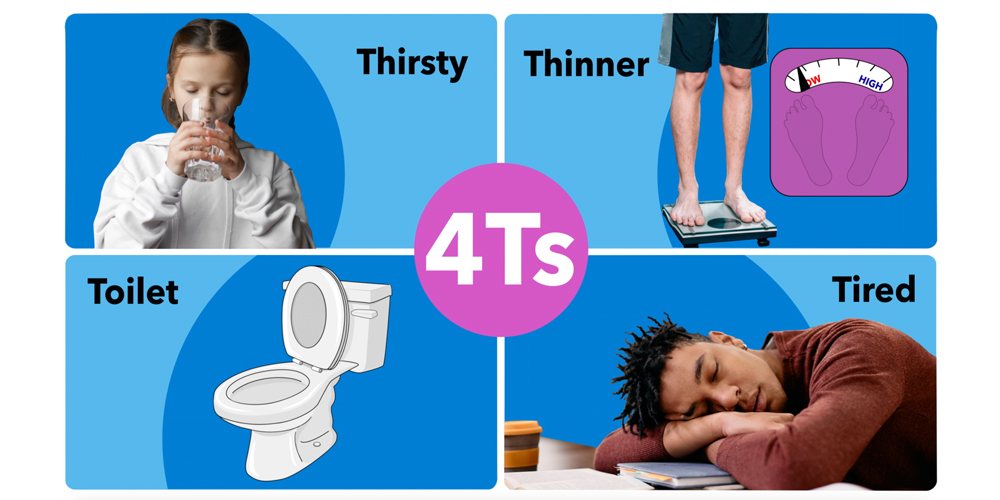
Type 1 Awareness
Parents, Carers, Family & Community
HCP Resources & Written Guidance
Who we help
Parents, Family & Friends
Schools & Teachers
Healthcare Professionals
Our Partnerships